Pre-Authorisation
Revolutionise customer experience with a game-changing approach to pre-authorisation
Revolutionise patient care and eliminate laborious and manual tasks with our game-changing solution to pre-authorisation. We think outside the box so you can put a tick in it. Quickly and securely validate and verify patients for treatments.
Doing it differently
Pre-authorisation is an essential part of the billing process. It is also one of the greatest hindrances to efficiency. But there is good news. For both insurers and hospitals. Pre-authorising eligible patients for treatment needn’t be complex.
Conquer previous authorisation challenges. By adopting our automated solution, you can wave goodbye to time-consuming and tedious manual processes. It’s a game changer. For you, as well as for the patients.
Simply choose the level of pre-authorisation to suit your business.
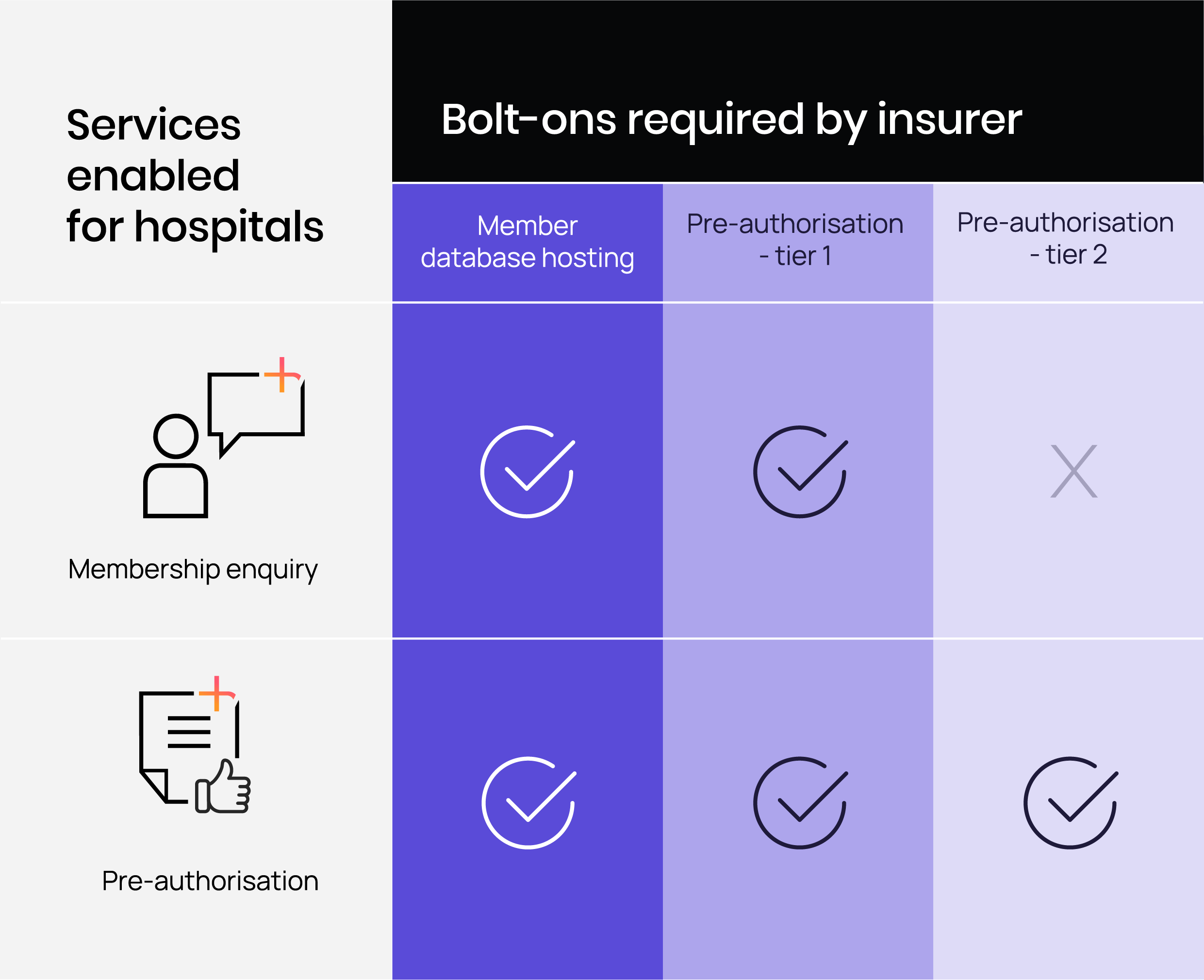
Improve efficiency
We help you to work smarter. Cut the complexity of managing authorisations and pre-treatment membership checks. Avoid the possibility of human errors. Get approval for all procedures in one online transaction. Deliver timely care.
Enhance customer experience
Long winded processes and lengthy phone calls are a thing of the past. Yes, it’s true. Automated systems will save costs for you. But showing people you care about their experience. That’s priceless.
Safe & secure
Safeguard your sensitive and personal patient data. You can now remove the need for manual submissions and information collection through insecure email or phone calls. Our secure platform gives the ultimate protection.
I’m ready to get started
News and Blogs
Appointment booking flows more smoothly over ICE
Want to know more about how ICE our online central booking system can benefit you? Learn more here.
Read full story about Appointment booking flows more smoothly over ICE“The whole process flows really well and it works for everyone” – Henry Muscatt, Schoen Clinic
From online invoicing to pre-authorisation and membership enquiry, Henry Muscatt, Schoen Clinic’s Finance and Revenue Assurance Manager, tells us why it’s just as important for award-winning hospitals to use our solutions as well as offering excellent clinical care.
Read full story about “The whole process flows really well and it works for everyone” – Henry Muscatt, Schoen ClinicWorking smarter with technology
It can be a shock to discover how much time is taken up by admin and business tasks in private practice.
Read full story about Working smarter with technology
